Diabetes and Foot Health: Preventing Ulcers, Deformities, and Amputation
Diabetes affects more than 25 million Americans, with millions more living with the condition undiagnosed. According to national data, Type 2 diabetes accounts for approximately 90–95% of all cases and is largely driven by insulin resistance, obesity, aging, and sedentary lifestyles. As diabetes continues to rise, so do the serious complications that affect the feet and lower extremities.
How Diabetes Affects the Feet
Diabetes can lead to multiple systemic health issues, including heart disease, stroke, high blood pressure, kidney disease, vision loss, and nerve damage. One of the most common and dangerous complications is peripheral neuropathy, a condition that causes loss of sensation in the feet.
When sensation is reduced, patients may not feel pain, pressure, cuts, or irritation on the bottoms of their feet. This makes it easy for minor problems to go unnoticed and progress into serious injuries.
Another major concern is poor circulation. Diabetes can reduce blood flow to the feet, limiting the body’s ability to heal wounds. Even small cuts or pressure points can develop into chronic foot ulcers that are slow to heal and prone to infection.
Diabetic Foot and Leg Ulcers
Studies show that up to 15% of people with diabetes will develop a serious foot ulcer during their lifetime. These ulcers often begin with repetitive pressure or friction that goes unnoticed due to neuropathy. Over time, calluses form and break down into open wounds.
Diabetic foot ulcers are a serious medical concern:
-
More than 50% of foot ulcers become infected
-
Many infections require hospitalization
-
One in five infected ulcers leads to amputation
-
Diabetes is responsible for approximately 80% of non-traumatic lower-limb amputations in the United States
Early detection and proper treatment are critical to reducing these risks.
The Importance of Early Detection and Daily Foot Care
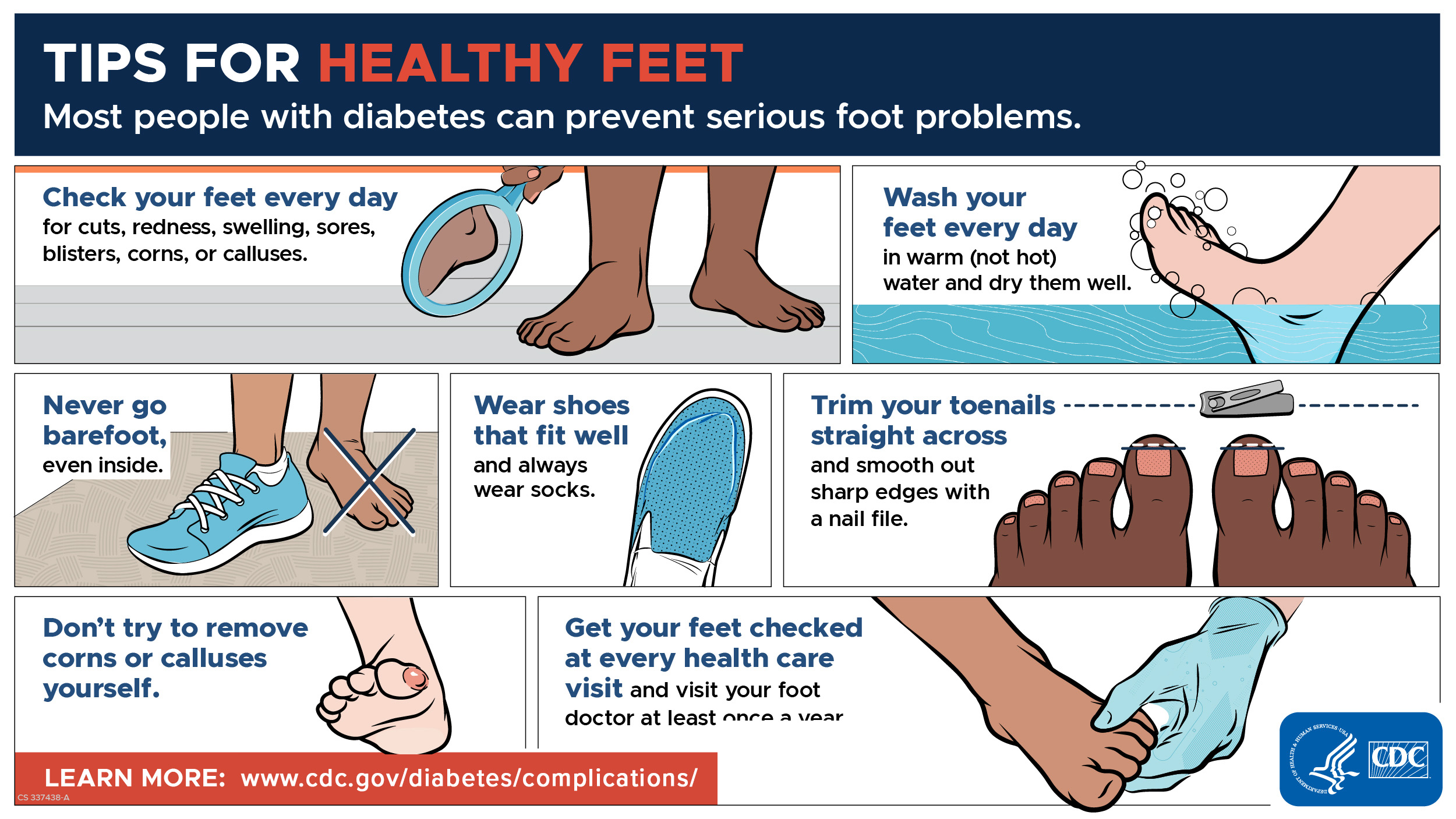
Preventing diabetic foot complications starts with awareness and consistency. Patients living with diabetes should:
-
Inspect their feet daily for cuts, redness, swelling, or drainage
-
Wear properly fitting shoes that minimize pressure points
-
Avoid walking barefoot
-
Maintain blood sugar levels within recommended ranges
-
Seek prompt care for any foot changes
Routine visits with a foot and ankle specialist allow for early identification of risk factors, reinforcement of self-care habits, and timely intervention before serious complications develop.
Foot and Ankle Deformities in Diabetes
Long-standing diabetes can lead to structural changes in the feet. These changes may include limited joint motion, muscle weakness, reduced sensation, and loss of protective fat padding. Together, these issues increase pressure on certain areas of the foot, making ulcers more likely.
One common example is hammertoe deformity, which can occur when diabetes-related muscle atrophy alters toe alignment. Increased pressure on the toes can result in skin breakdown and ulcer formation.
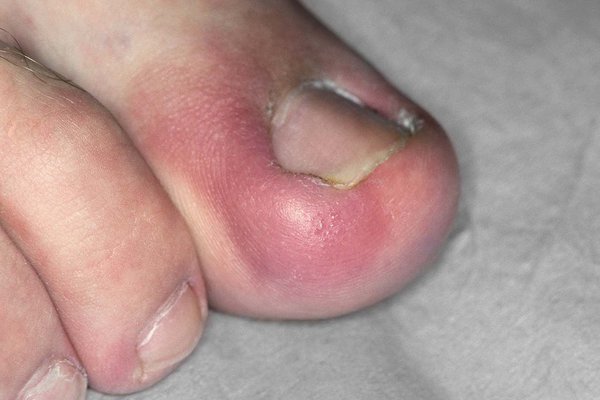
Another serious condition is Charcot neuroarthropathy (Charcot foot). This condition typically affects patients with diabetes and neuropathy. Early signs may include a foot that is warm, red, swollen, and sometimes painful. As the condition progresses, the bones weaken, fracture, and collapse, leading to severe foot deformity and instability.
Treatment Options for Diabetic Foot Conditions
Treatment focuses on reducing pressure, promoting healing, preventing infection, and preserving foot structure.
Conservative treatments may include:
-
Custom orthotics and diabetic shoes
-
Bracing to offload pressure
-
Strict blood glucose control
-
Wound care and infection management
For chronic or non-healing ulcers, advanced therapies such as bioengineered skin substitutes may be used to stimulate healing by providing growth factors and structural support.
Treating Charcot Foot Deformity
Charcot foot often requires an extended period of non-weightbearing immobilization using casts or specialized braces to prevent further collapse. In some cases, surgical treatment may be necessary.
Surgical options may include:
-
Ostectomy procedures to relieve pressure causing ulcers
-
Reconstructive surgery to realign and stabilize the foot
The goal of treatment is to restore stability, prevent ulcer recurrence, and reduce the risk of infection or amputation.
When to See a Foot and Ankle Specialist
Foot pain, numbness, swelling, wounds, or changes in foot shape are not normal and should never be ignored—especially for individuals with diabetes. Early evaluation and ongoing foot care can dramatically reduce the risk of ulcers, infections, and limb loss.
If you are living with diabetes, regular foot exams and prompt treatment of any concerns are essential to protecting your long-term health and mobility.
Written for patient education and awareness by a foot and ankle care specialist.
David Auguste, DPM, Diplomat of American Board of Podiatric Medicine
You might also like
Benefits of Medical Pedicures.
It’s Time to Schedule Yours A medical pedicure at Ankle & Foot Associates provides clinical-grade foot care in a sterile…